Creating Access to Healthy Food and Stable Housing

We’ve been spending a few months looking closely at how data can help improve outcomes and reduce costs in community health care. Today, we’ll look at two crucial components in improving community health: access to healthy food and stable housing.
Increasing Access to Health Foods
Obesity is associated with the leading causes of death in the U.S., as it is a precursor to diabetes, heart disease, stroke, and some types of cancer. The estimated annual health care costs of these obesity-related illnesses are “a staggering $190.2 billion or nearly 21% of annual medical spending in the United States.”
As a result, finding ways to help reduce the obesity rate in communities with poor socio-economic conditions has gained growing importance, particularly for Medicaid providers. Genetics, family lifestyle and the built environment all contribute to the obesity epidemic. The built environment can include the presence of sidewalks, good access to transit, parks and playgrounds, as well access to fresh, healthy foods.
A lack of access to healthy food can contribute to poor nutrition, higher levels of obesity and other diet-related diseases. Metrics are available to determine where at-risk populations lack access to fresh foods, and they are enabling states and providers to pinpoint opportunities for partnerships or support development that will bring better food choices into neighborhoods.
In Massachusetts, health care providers successfully partnered with restaurants, school food services providers, and others to provide healthy food options to reduce obesity. This type of partnership could be replicated elsewhere.
In Atlanta, 30% of all adults are reported to be obese. There are parts of Atlanta where the obesity rate is higher than 40% and where access to a supermarket, with fresh food, is limited. These are places where collaborations between health organizations and the private sector to bring fresh food to the area can help to improve health outcomes of the people who live there.
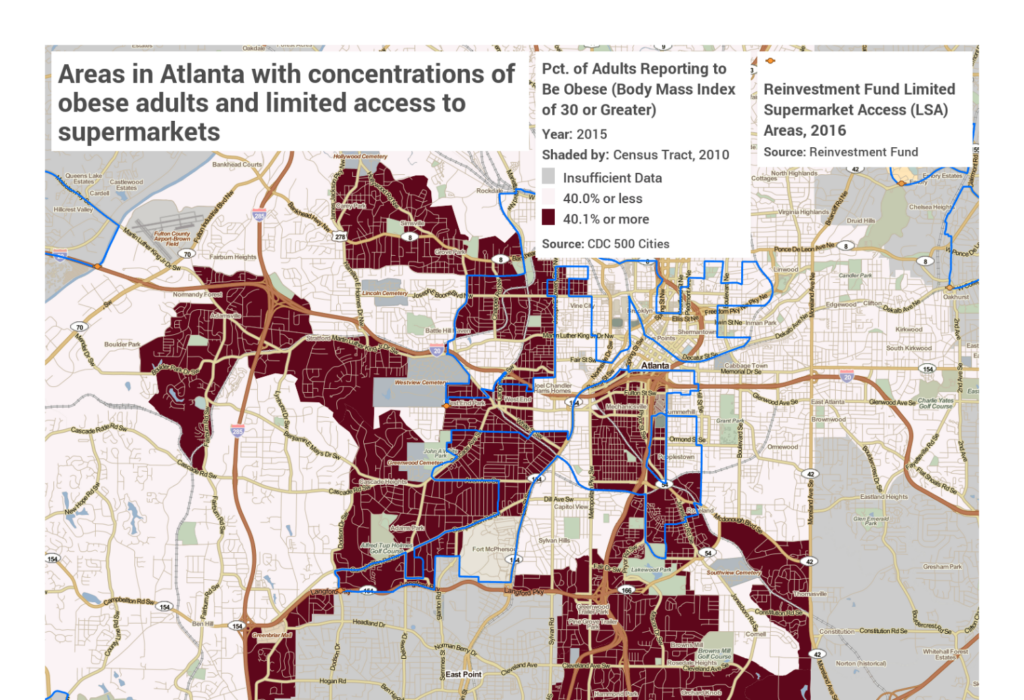
Connecting Housing Stability and Health
Housing stability is recognized as highly important to an individual’s long-term health. Those who have lower incomes and are burdened by the expense of a home or apartment, those who live in substandard housing conditions, those who are homeless, and those who have reached an age at which living independently is a challenge have reduced chances of good long-term health.
The financial stress or the fragile nature of those with unstable living conditions can make caring for their health overwhelming and unmanageable. After returning home from a hospital stay, for example, hospital readmission rates are high as patients do not always have the supports needed at home to heal. As a result, hospitals are creating partnerships with local support services or housing providers to better ensure the long-term success of patients. Philadelphia, Boston, Phoenix and Los Angeles are among numerous cities working on initiatives designed to bridge this housing and health care gap.
Opportunities for collaborations in Houston can be visualized on a map. In areas where more than 41% of households are severely burdened by the cost of renting a home (darkest green areas), health care organizations can identify non-profit housing agencies (orange squares) working in those areas for potential collaboration on coordinating hospital release support services.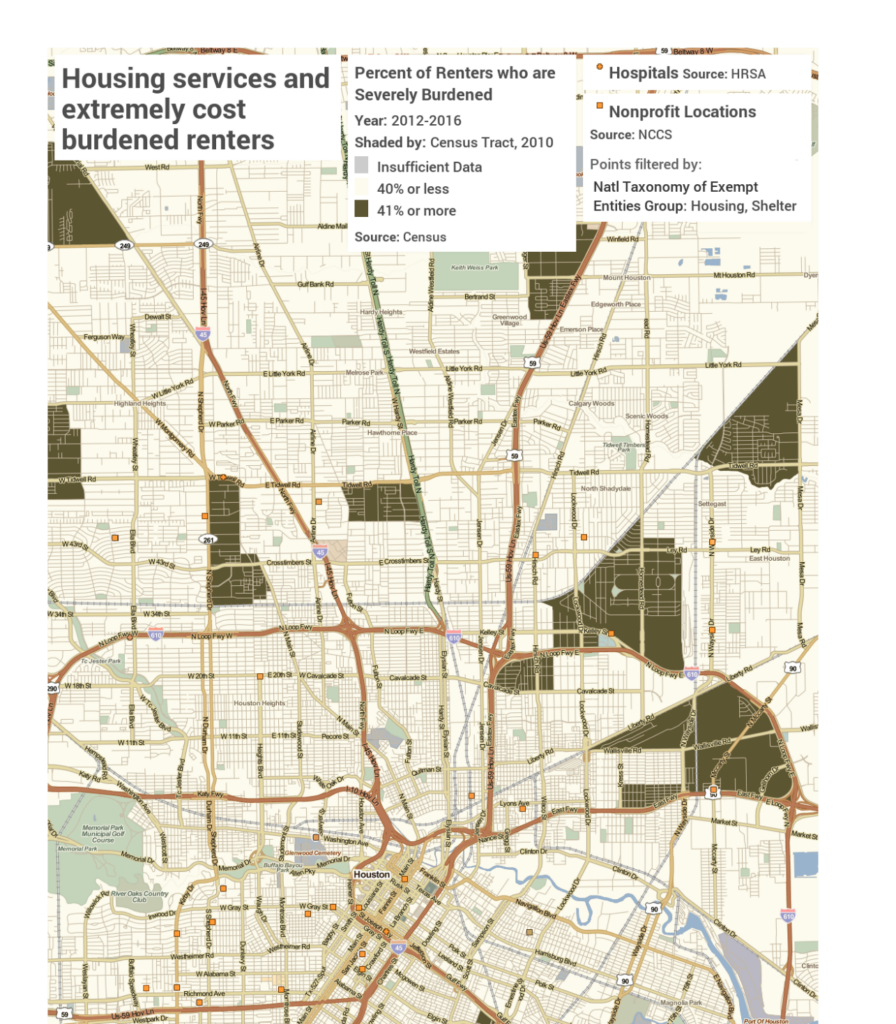
This post was adapted from our recent white paper, “Do Our Zip Codes Need to Determine Our Health?” You can download the complete paper here.